This clinical guide helps The Woodlands patients move beyond marketing claims to evaluate regenerative medicine based on diagnosis, safety, and realistic outcomes. It emphasizes the importance of understanding tissue physiology and asking specific questions during consultations.
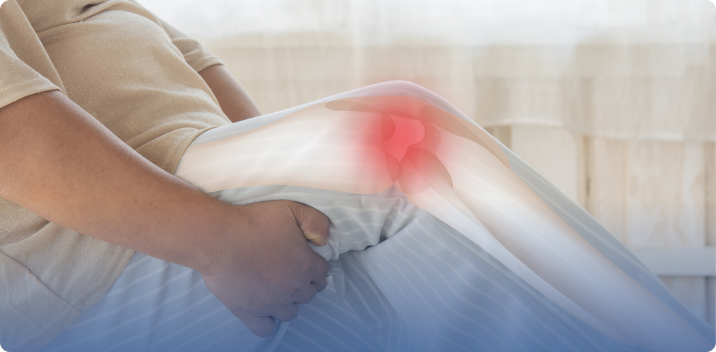
Stem cell therapy generates significant interest among patients seeking alternatives to surgery and long-term medication for joint degeneration, soft tissue injuries, and inflammatory conditions. For patients in The Woodlands, TX, the critical step is moving past marketing claims and evaluating the therapy through a clinical lens that accounts for evidence, candidacy, realistic outcomes, and provider qualifications. This guide provides the framework for that evaluation.
What Makes Stem Cell Therapy Different from Other Treatments?
Stem cell therapy introduces biological cells with regenerative potential directly into damaged tissue, aiming to support repair rather than simply manage symptoms. This distinguishes it from treatments that mask pain (injections, medications) or replace structures entirely (surgery).
The cells used in stem cell therapy have the ability to differentiate into multiple tissue types and secrete growth factors, cytokines, and signaling molecules that recruit the body's own repair mechanisms. This paracrine signaling effect may be as important as the cells themselves.
Sources of stem cells used clinically include:
- Bone marrow aspirate concentrate (BMAC): Harvested from the patient's own iliac crest, providing autologous mesenchymal stem cells and growth factors
- Adipose-derived stem cells: Extracted from the patient's fat tissue through a minimally invasive procedure
- Umbilical cord-derived products: Allogeneic products from donated birth tissue containing mesenchymal stem cells, growth factors, and extracellular matrix proteins
Each source has different cell concentrations, processing requirements, and clinical applications. The choice of cell source should be driven by the clinical indication, not by which product a clinic happens to carry.
How Should You Evaluate Whether You Are a Candidate?
Candidacy for stem cell therapy depends on a matrix of factors, not just the presence of pain or degeneration:
Severity of damage: Stem cells work best in an environment where residual tissue structure provides scaffolding for repair. Mild to moderate degeneration responds better than end-stage damage where structural integrity is lost.
Location and type of tissue: Cartilage, tendons, ligaments, and certain soft tissues have demonstrated responsiveness to stem cell therapy. Some tissues heal more predictably than others.
Overall health status: Patients with uncontrolled diabetes, active autoimmune flares, or systemic infection are generally not candidates until those conditions are stabilized. The body's ability to utilize stem cells depends on a functional metabolic and immune environment.
Prior treatment history: Understanding what has and has not worked helps set appropriate expectations. Patients who have failed conservative care but are not yet surgical candidates often represent the ideal treatment window.
Realistic expectations: Patients who understand that stem cell therapy supports repair rather than guarantees complete regeneration tend to have better satisfaction with outcomes, even when results are partial.
A provider who performs a thorough evaluation including imaging review, physical examination, and candid discussion of alternatives demonstrates the clinical rigor this therapy requires.
What Does the Evidence Actually Support?
The evidence base for stem cell therapy is substantial and growing, but varies by application:
Strong evidence:
- Knee osteoarthritis: Multiple randomized trials showing pain reduction and functional improvement, particularly in mild to moderate disease
- Rotator cuff repair augmentation: Studies showing improved healing rates when stem cells supplement surgical repair
Moderate evidence:
- Hip osteoarthritis: Positive case series and emerging trial data
- Tendon injuries: Growing evidence for conditions including Achilles tendinopathy and lateral epicondylitis
- Disc degeneration: Early but promising data for intradiscal injections
Early or limited evidence:
- Neurological conditions, cardiac repair, autoimmune diseases
- These applications are primarily in the research phase
Patients should be cautious of clinics claiming stem cell therapy cures conditions that lack clinical evidence. The therapy shows genuine promise for musculoskeletal applications where the evidence is strongest, and that is where clinical focus should remain.
What Red Flags Should You Watch for When Choosing a Provider?
The stem cell therapy landscape includes both qualified clinicians and predatory marketers. Red flags include:
- Guaranteed outcomes: No legitimate provider can guarantee stem cell therapy results
- One-size-fits-all pricing and protocols: If every patient receives the same treatment regardless of condition, the approach lacks clinical individualization
- No imaging or diagnostic workup: Stem cells injected without knowing exactly what you are treating is clinically indefensible
- Pressure to commit immediately: High-pressure sales tactics including limited-time pricing or seminar-based enrollment suggest marketing over medicine
- No follow-up plan: If the provider does not include structured follow-up testing and rehabilitation, the treatment plan is incomplete
- Claims about treating dozens of unrelated conditions with the same stem cell product
Qualified providers take time to evaluate, diagnose precisely, discuss alternatives honestly, and track outcomes systematically. The consultation should feel like a medical evaluation, not a sales presentation.
How Do You Measure Whether Stem Cell Therapy Worked?
Measuring outcomes requires established benchmarks before treatment and systematic reassessment afterward:
- Pain scales: Validated instruments like the Visual Analog Scale (VAS) or Numeric Rating Scale
- Functional assessments: Condition-specific scores such as WOMAC for knee osteoarthritis or DASH for upper extremity conditions
- Imaging: Follow-up MRI or ultrasound at 6 to 12 months to assess tissue changes
- Activity milestones: Return to specific activities that were limited before treatment
- Medication reduction: Decreased reliance on pain medications or anti-inflammatories
Progress typically follows a gradual curve with initial improvements around 4 to 8 weeks and continued gains over 3 to 12 months. The best outcomes occur when patients complete rehabilitation protocols that strengthen the repaired tissue and restore functional capacity.
What Role Does Rehabilitation Play After Stem Cell Treatment?
Rehabilitation is not optional after stem cell therapy. The biological repair process requires appropriate mechanical loading to produce functional tissue rather than scar tissue.
Weeks 1-2: Rest and protection of the treated area. Minimal loading to allow the injected cells to establish in the target tissue.
Weeks 2-6: Gradual introduction of controlled movement and light loading. The goal is stimulating the repair process without overwhelming newly forming tissue.
Weeks 6-12: Progressive strengthening and functional exercises. Tissue remodeling responds to mechanical demand during this critical window.
Months 3-6: Return to full activity with continued conditioning. Most patients achieve their peak improvement during this period.
Skipping rehabilitation is one of the most common reasons patients report disappointing outcomes from stem cell therapy. The cells provide the biological foundation; rehabilitation provides the mechanical stimulus that shapes functional tissue.
Clinical Stem Cell Evaluation at Prince Health in The Woodlands
If you are considering stem cell therapy and want an honest, evidence-based evaluation of whether it fits your specific condition, Prince Health provides the clinical framework for informed decision-making.
Prince Health and Wellness is located at 10847 Kuykendahl Rd #350, The Woodlands, TX. Our stem cell therapy evaluation includes imaging review, physical examination, discussion of alternatives, and transparent information about expected outcomes, costs, and the rehabilitation commitment required. We believe every patient deserves complete information before committing to treatment.
Frequently Asked Questions
How much does stem cell therapy cost in The Woodlands?
Stem cell therapy typically ranges from $3,000 to $8,000 per treatment area, depending on the cell source, processing requirements, and complexity of the case. Insurance does not generally cover stem cell therapy. Prince Health provides detailed pricing during consultation and can discuss payment options including HSA and FSA eligibility.
Is stem cell therapy painful?
The procedure itself involves local anesthesia at the injection site, making it well tolerated by most patients. Bone marrow aspiration from the iliac crest causes brief discomfort during the draw. Post-procedure soreness at the injection site typically lasts 2 to 5 days and is managed with ice and mild analgesics. The discomfort is significantly less than surgical recovery.
How many stem cell treatments do I need?
Most patients receive one to two treatments, with reassessment at 3 to 6 months to determine whether additional therapy is warranted. The number depends on the severity of the condition, the cell source used, and the individual healing response. Some conditions respond fully after a single treatment, while others benefit from a second session.
Can stem cell therapy help with back pain?
Stem cell therapy shows promising early evidence for disc degeneration and facet joint pain. Intradiscal stem cell injections aim to support disc repair and reduce inflammation. Candidacy depends on the specific cause and severity of back pain, and not all back conditions are appropriate for this approach. A thorough diagnostic evaluation determines suitability.
What is the difference between stem cell therapy and PRP?
PRP uses concentrated growth factors from your blood to stimulate healing, while stem cell therapy introduces regenerative cells capable of differentiating into tissue types. PRP is often the first-line regenerative approach for mild conditions due to its lower cost and strong evidence base. Stem cell therapy is typically considered for more significant tissue damage or when PRP has not produced sufficient improvement.